Ulcerative colitis
Эпидемиология. Заболеваемость
В последние годы отмечается рост числа случаев воспалительных заболеваний кишечника (колитов) в северно-
В Западной Европе и США ежегодно заболевает от 3, 5-6, 5 больных на 105 населения до 60 больных на 105 населения. Более 50% больных имеют возраст 20-40 лет, средний возраст в момент возникновения болезни составляет 29 лет. Европейский комитет в 1991-1992г. провел эпидемиологическое исследование распространенности язвенного колита в странах ЕС (участвовало 20 стран). Частота выявления на 100тыс. населения составило 5,8; городское и сельское население – поровну.
Поданным M.H. Vatn и др. (Норвегия) частота НЯК увеличивается:
1976 -
Этиология
До настоящего времени не существует единого мнения о причинах возникновения и механизмах развития НЯК. Выделяют следующие основные факторы.
Этиологические факторы:
- Генетический фактор ( система HLA: обнаружены генетические HLA-
маркеры НЯК, БК в различных популяциях; с помощью HLA – ДНК генотипирования выявлены маркеры предрасположенности и устойчивости к НЯК (аллель DRB1*01 ген. маркер предрасположенности к началу заболевания в молодом возрасте, аллель DRB1*08 ассоциирован с дистальными формами и возникновением болезни в возрасте 30- 49 лет). - Микробный фактор ( высокая степень иммунизации больных НЯК 0-
антигеном Esherichia Coli 014; E.Coli обладает высокой адгезивной способностью к эпителиальным клеткам слизистой оболочки и может инициировать их разрешение; положительное дейсnвие пробиотиков содержащих Esherichia сoli- штамм Nissle 1917) - Нарушение проницаемости кишечного барьера.
- Факторы окружающей среды (Никотин: у злостных курильщиков НЯК встречается реже, чем у некурящих, при БК курение в несколько раз увеличивает риск заболевания; лекарственные препараты: НПВП; нерациональное питание: значительный рост данной патологии в странах, где в рационе используют «fast foods».
- Нарушение иммунного ответа (нарушения регуляции местного иммунного ответа лежит в основе развития воспалительной реакции в стенке кишки)
Таким образом, генетическая предрасположенность, возможности иммуного ответа , воздействие єкзогенных факторов при наличии ряда эндогенных нарушений приводит к развитию хронического воспаления слизистой оболочки при неспецифическом язвенном колите (НЯК
Патогенез
В развитии воспаления при язвенном колите задействованы многочисленные механизмы тканевого и клеточного повреждения. Бактериальные и тканевые антигены вызывают стимуляцию Т- и В-лимфоцитов. При обострении язвенного колита обнаруживается дефицит иммуноглобулинов, что способствует проникновению микробов, компенсаторной стимуляции В-клеток с образованием иммуноглобулинов М и G. Дефицит Т-супрессоров приводит к усилению аутоиммунной реакции. Усиленный синтез иммуноглобулинов М и G сопровождается образованием иммунных комплексов и активацией системы комплемента, который обладает цитотоксическим действием, стимулирует хемотаксис нейтрофилов и фагоцитов с последующим выделением медиаторов воспаления, которые и вызывают деструкцию эпителиальных клеток. Среди медиаторов воспаления, прежде всего следует назвать цитокины IL-1Я, IF-y, IL-2, IL-4, IL-15, которые влияют на рост, движение, дифференциацию и эффекторные функции многочисленных клеточных типов, вовлеченных в патологический процесс при язвенном колите. Помимо патологических иммунных реакций, повреждающее действие на ткани оказывают активный кислород и протеазы; отмечается изменение апоптоза, т. е. механизма клеточной смерти.
Важная роль в патогенезе язвенного колита отводится нарушению барьерной функции слизистой оболочки кишечника и ее способности к восстановлению. Считается, что через дефекты слизистой оболочки в более глубокие ткани кишки могут проникать разнообразные пищевые и бактериальные агенты, которые затем запускают каскад воспалительных и иммунных реакций.
Большое значение в патогенезе язвенного колита и провокации рецидива заболевания имеют особенности личности больного и психогенные влияния. Индивидуальная реакция на стресс с аномальным нейрогуморальным ответом может явиться пусковым механизмом развития болезни. В нервно-психическом статусе больного язвенным колитом отмечаются особенности, которые выражаются в эмоциональной нестабильности.
Патоморфология
Поражение начинается чаще всего от прямой кишки - зубчатой линии и распространяется в проксимальном направлении. На ранних стадиях колита отмечают сосудистую реакцию с дальнейшим нарушением целостности эпителия, присоединением изъязвлений слизистой оболочки. Возникающие язвы захватывают только подслизистый слой, в глубину стенки кишки как правило не распространяются. В активную фазу язвы разного размера распространяются на отечной, полнокровной слизистой оболочке.
Иногда она представляет собой сплошную язвенную поверхность, покрытую пленкой фибрина. Но чаще всего на слизистой оболочке отмечают большое количество мелких эрозий и язв, в том числе псевдополипов, развитие которых связывают с деструкцией слизистой оболочки, регенерацией эпителия. Тяжесть морфологических изменений нарастает в дистальном направлении (наиболее выражены в нисходящей и сигмовидной кишке). В 18-30% может поражаться терминальный отдел подвздошной кишки.
На ранней стадии болезни и при ее обострении в воспалительном инфильтрате преобладают лимфоциты, при длительном течении – плазматические клетки и эозинофильные гранулоциты. Эти клетки выявляют в области дна язв, как и покрытую фибрином грануляционную ткань.
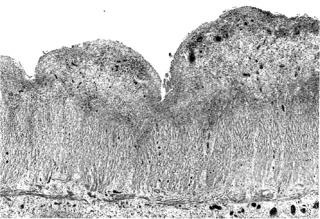
Воспалительным процессом поражены все слои кишечной стенки.
Классификация НЯК
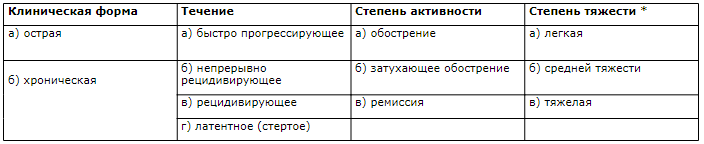
Анатомическая характеристика
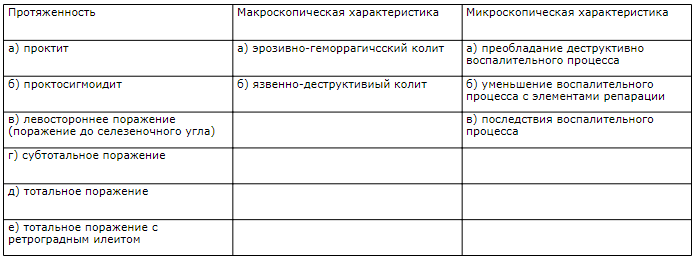
По степени тяжести

По эндоскопической картине выделяют четыре степени активности воспаления в кишке: минимальная, умеренная, выраженная и резко выраженная.
I степень (минимальная) характеризуется отеком слизистой оболочки, гиперемией, отсутствием сосудистого рисунка, легкой контактной кровоточивостью, мелкоточечными геморрагиями.
II степень (умеренная) определяется отеком, гиперемией, зернистостью, контактной кровоточивостью, наличием эрозий, сливными геморрагиями, фибринозным налетом на стенках.
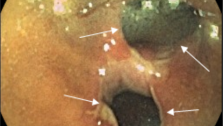
III степень (выраженная) характеризуется появлением множественных сливающихся эрозий и язв на фоне описанных выше изменений в слизистой оболочке. В просвете кишки гной и кровь.
IV степень (резко выраженная), кроме перечисленных изменений, определяется формированием псевдополипов и кровоточащих грануляций.
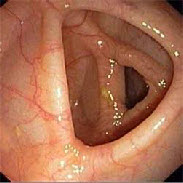 Нормальная слизистая оболочка толстой кишки
Нормальная слизистая оболочка толстой кишки
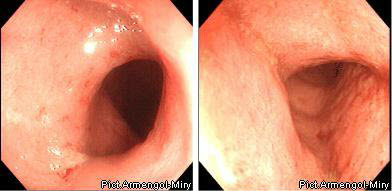 І степень
І степень
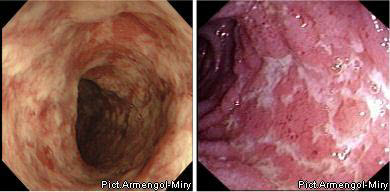 ІI степень
ІI степень
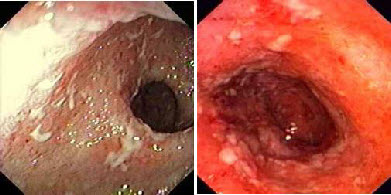 ІII степень
ІII степень
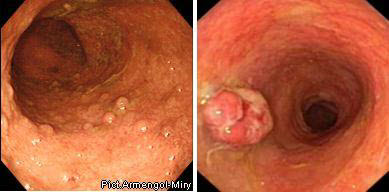 ІV степень
ІV степень
Эндоскопический индекс Рахмилевича (1989)
1. Рассеивающие свет грануляции на поверхности слизистой оболочки (зернистость): нет - 0, есть - 2.
2. Сосудистый рисунок: нормальный - 0, деформированный или размытый - 1, отсутствует - 2.
3. Кровоточивость слизистой оболочки: отсутствует - 0, небольшая контактная - 2, выраженная (спонтанная) - 4.
4. Повреждения поверхности слизистой оболочки (эрозии, язвы, фибрин, гной): отсутствуют - 0, умеренно выражены - 2, значительно выражены.
В настоящее время наиболее распространенной оценкой степени тяжести и активности НЯК является ее определение по Schroeder или клиники Mayo.
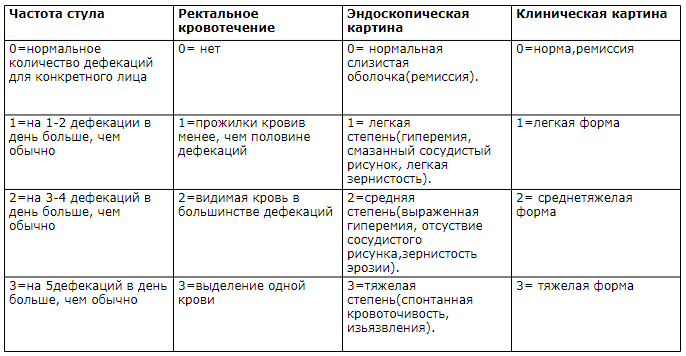
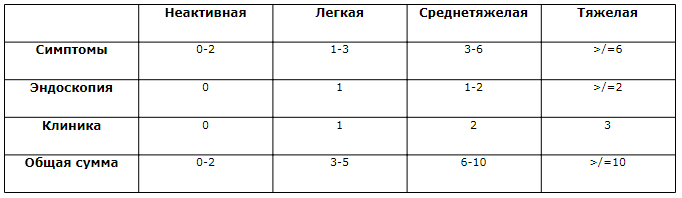
Клиническая картина
НЯК всегда начинается с поражения слизистой прямой, сигмовидной кишки в 90-95% случаев. При язвенном колите отмечается не только поражение толстого кишечника, но и различных органов и систем.
Характерными клиническими симптомами при неспецифическом язвенном колите (НЯК), чаще всего является частый жидкий стул, что связано с ускоренным продвижением кишечного содержимого, усилением поступления в просвет кишки экссудата, транссудата, выделяемого воспаленной слизистой оболочкой; также ведущим симптомом является кровотечение. Большие кровопотери связаны с активным некротическим процессом и крупными язвенными дефектами в слизистой оболочке толстой кишки, распространением процесса на большую часть органа. Выделение крови у больных НЯК не всегда носит обязательный характер.
Иногда заболевание может начинаться с болей в животе, запоров.
Основные клинические симптомы неспецифического язвенного колита (НЯК).

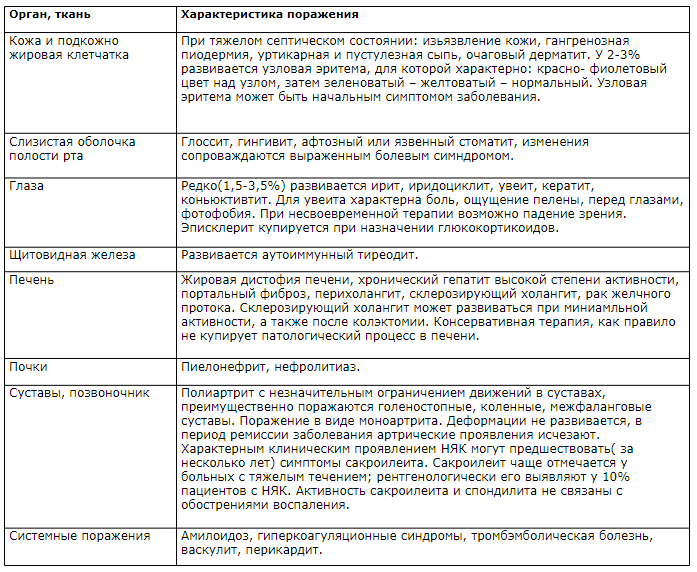
В ряде случаев эти поражения могут предшествовать появлению кишечных симптомов. Внекишечные проявления наблюдаются у больных юношеского возраста реже, чем в более старшем возрасте.
Осложнения при НЯК
При язвенном колите наблюдаются разнообразные осложнения, которые можно разделить на местные и системные.
Местные осложнения:
- Токсическая дилятация толстой кишки развивается в 3-
5% случаев. Развиавется чрезмерное расширение толстой кишки, которому способствуют стриктуры дистальных отделов, поражение нервно- мышечного аппарата, интоксикация. Летальность в случае развития этого осложнения составляет 28- 32%. - Перфорация толстой кишки возникает приблизительно в 3-
5% случаев и часто приводит к смерти (72- 100%). - Стриктуры прямой или толстой кишки (3-
19 % случаев). Как правило развиваются на небольшом (2- 3см.) протяжении толстой кишки при длительности болезни более 5 лет; приводят к развитию клиники кишечной непроходимости. - Кишечное кровотечение (1-
6% случаев). Причиной является васкулит, некроз стенки сосудов, а также флебит, разрыв расширенных вен. - Перианальные осложнения (4-
30% случаев): парапроктиты, свищи, трещины, перианальные раздражения кожи. - Рак толстой кишки. НЯК считается предраковым заболеваниям. Риск развития рака толстой кишки повышается по мере увелечения длительности течения болезни с левосторонней локализацией, субтотальным и тотальным поражением.
- Воспалительные полипы. Выявляют менее чем у половины больных с НЯК. Полипы требуют проведения биопсии, гистологического исследования.
Острая токсическая дилатация толстой кишки — одно из самых опасных осложнений язвенного колита. Токсическая дилатация характеризуется расширением сегмента или всей пораженной кишки во время тяжелой атаки язвенного колита. Характерно снижение частоты дефекаций, усиление болей в животе, нарастание симптомов интоксикации ( заторможенность, спутанность сознания), повышение температуры тела (до 38-39 *С). При пальпации тонус передней брюшной стенки снижен, пальпируется резко расширенный толстый кишечник, перистальтика резко ослаблена. Больные с токсической дилатацией толстой кишки на начальных стадиях нуждаются в интенсивной консервативной терапии. При ее неэффективности выполняется оперативное вмешательство.
Перфорация толстой кишки является наиболее частой причиной смерти при молниеносной форме язвенного колита, особенно при развитии острой токсической дилатации. Вследствие обширного язвенно-некротического процесса стенка толстой кишки истончается, теряет свои барьерные функции и становится проницаемой для разнообразных токсических продуктов, находящихся в просвете кишки. Помимо растяжения кишечной стенки решающую роль в возникновении перфорации играет бактериальная флора, особенно кишечная палочка с патогенными свойствами. При обзорной рентгеноскопии в брюшной полости выявляют свободный газ. В сомнительных случаях прибегают к Лапароскопии.
Массивные кишечные кровотечения встречаются сравнительно редко и как осложнение представляют собой менее сложную проблему, чем острая токсическая дилатация толстой кишки и перфорация. У большинства больных с кровотечением адекватная противовоспалительная и гемостатическая терапия позволяют избежать операции. При продолжающихся массивных кишечных кровотечениях у больных язвенным колитом показано оперативное вмешательство.
Риск развития рака толстой кишки при язвенном колите резко возрастает при длительности заболевания свыше 10 лет, если колит начался в возрасте моложе 18 . В первые 10 лет воспалительного заболевания кишечника колоректальный рак возникает в 1% случаев, через 20 лет – в 7%, через 30 лет – в 16% через 40лет - в 53% случаев (Хендерсон Дж.М.2005(ред)).
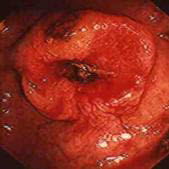
Стриктуры прямой или толстой кишки. Непроходимость вызванная стриктурами доброкачественного генеза встречается приблизительно у 10% больных с неспецифическим язвенным колитом (НЯК). У трети этих пациентов препятствие локализуется в прямой кишке. Необходимо проводить дифференциальную диагностику этих стриктур от колоректального рака и болезни Крона.
Общие осложнения.
- Амилоидоз.
- Гиперкоагуляцонные синдромы, анемия, тромбэмболическая болезнь, гипопротеинемия, нарушение водно-
электролитного обмена, гипокалиемия. - Васкулит, перикардит.
- Трофические язвы голеней и стоп.
- Полиартрит, ирит.
Диагностика НЯК
При диагностике необходимо учитывать данные анамнеза и физикального обследования, результаты дополнительных исследований (ректороманоскопия, колоноскопия, ирригоскопия, лабораторные данные).
В зависимости от остроты и тяжести проявлений заболевания, клинические находки у пациентов с язвенным колитом варьируют от нормы до клиники перитонита. При пальцевом исследовании прямой кишки можно выявить - перианальные абсцессы, свищи прямой кишки, трещины анального прохода, спазм сфинктера, бугристость и утолщение слизистой, ригидность стенки, наличие крови, слизи и гноя.
Эндоскопическое исследование толстой кишки (в острой фазе проводится без предварительной подготовки клизмами). Ректороманоскопия, колоноскопия являются одним из основных методов исследования, так как прямая кишка поражается в 95% случаев. Характерно наличие слизи, крови, гноя которые закрывают слизистую.
При исследовании отмечается: отек и гиперемия слизистой оболочки сигмовидной и прямой кишок; утрачивается сосудистый рисунок характерный для нормальной слизистой оболочки толстой кишки; исчезает гаустрация толстой кишки. Различные по величине и форме эрозии и язвы с подрытыми краями и дном покрытым гноем и фибрином. Наличие одиночной язвы должно настораживать в отношении рака. При длительном течение заболевания, в сохранившихся островках слизистой оболочки наблюдается отек и избыточная регенерация эпителия с образованием псевдополипов. НЯК лёгкой степени проявляется в виде зернистости слизистой оболочки.
Колоноскопия позволяет оценивать протяженность и тяжесть поражения, особенно при подозрении на наличие Малигнизации.
Противопоказаниями к ректороманоскопии и колоноскопии являются:
- Тяжелое течение неспецифического язвенного колита (НЯК).
- Токсический мегаколон.
- Подозрение на перфорацию, перитонит
Рентгенологические методы исследования
Рентгеноскопическое исследование органов брюшной полости используется не только для диагностики самого заболевания, но и его тяжелых осложнений, в частности острой токсической дилатации толстой кишки. При I степени дилатации увеличение диаметра кишки в ее самом широком месте составляет 8-10 см, при II — 10 - 14 см и при III — свыше 14см. При токсическом мегаколоне обнаруживается избыточное количество газа в расширенной ободочной кишке, потеря тонуса, уровни жидкости.
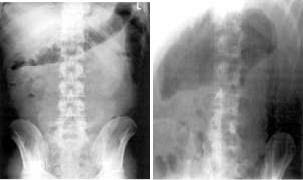
Ирригоскопия
Ирригоскопия является одним из основных диагностических методов НЯК, но в фазе обострения болезни она противопоказана.
Ранние рентгенологические проявления неспецифического язвенного колита (НЯК) включают: гиперкинезию, спазм отдельных сегментов кишки, умеренное утолщение, нечеткость контуров складок слизистой оболочки, «зернистую» слизистую оболочку, позже исчезают гаустры, становятся зубчатыми контуры кишки.
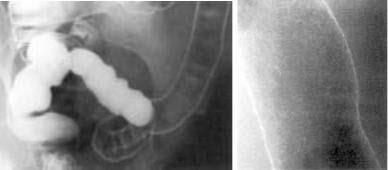
При тяжелом течении болезни выявляют:
- Пятнистость (мраморность) рисунка рельефа слизистой оболочки.
- Ригидность стенки.
- Отсуствие (деформация) гаустр.
- Нечеткость, неровность контуров.
- Неравномерное сужение или укорочение кишки.
- Множественные дефекты наполнения (псевдополипоз).
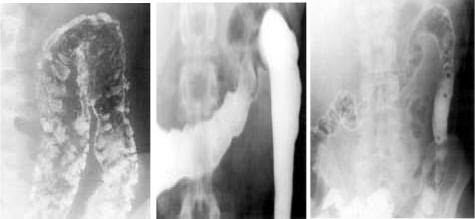
Лабораторные методы
У пациентов с язвенным колитом выявляются анемия и лейкоцитоз в различной степени, гипо- и диспротеинемия. Тяжелое течение болезни сопровождается гипокалиемией, снижением концентрации бикарбонатов в результате потери солей и жидкости через кишечник. Следствием хронической потери крови является истощение запасов железа. Синдром мальабсорбции, снижение синтетической функции печени приводят к гипоальбуминемии. Гипербилирубинемия, повышение активности ЩФ в сыворотке крови свидетельствует о сопутствующем холангите и перихолангите.
Микробиологическое исследование. Всем больным, у которых заболевание выявлено впервые, необходимо исключить инфекционную природу энтероколита. Выполняются мазки и посевы кала для исключения колита вирусной этиологии, хламидиоза, патогенной флоры и паразитарных поражений. Изменения облигатной микрофлоры, снижение положительных находок Lactobacillus bifidus до 61% (у здоровых до 98%), резкое возрастание молочнокислых, кишечных, палочек и энтерококков. Значительные изменения в составе микробов факультативной группы - рост патогенных стафилококков (превышает их содержание по сравнению с нормой в 60 и более раз) протея. Обязательным является определение чувствительности микрофлоры к антибиотикам. Патоморфологическое исследование. В основном наблюдается поражение слизистой оболочки, язвы проникают до подслизистого слоя, реже до мышечного слоя. Их края ровные, подрытые. В части случаев в сохранившихся участках слизистой оболочки возникает избыточная регенерация железистого эпителия с образованием псевдополипов. Является характерным наличие “крипт-абсцессов”.
Ультрасонография. Применяется интестинальная транскутанная и эндосонография. Особенно метод полезен, где выявлены противопоказания к эндоскопии, ирригоскопии. По данным W.B.Schwerk чувствительность и специфичность чрескожной сонографии равна 90,3 и 88,4% соответственно. При панколите и левостороннем колите 94 и100%, при ректосигмоидном поражении – только 50%. Большое значение имеет доплероангиография. Компьютерная томография с применением контраста внутривенно или после приема через рот. Метод позволяет опредилить толщину стенки кишки, абсцесса брюшной полости, стриктуры, опухоли.
МРТ Высокорезультативный метод для оценки воспаления стенки кишки особенно при введении контраста с добавлением метилцелюллозы.
Позитрон- эмиссионная томография с мечеными технецием 99 лейкоцитами.
Дифференциальный диагноз.
Дифференциальная диагностика должна проводиться с целым рядом нозологических форм, включающих инфекционные, функциональные и злокачественные болезни. Первая атака язвенного колита может протекать под маской острой дизентерии. Правильной диагностике помогают данные ректороманоскопии и бактериологического исследования. Сальмонеллез нередко симулирует картину язвенного колита, так как протекает с диареей и лихорадкой, но в отличие от него кровавая диарея появляется только на 2-й неделе болезни. Из других форм колита инфекционного генеза, требующих дифференциации от язвенного, следует отметить:
1. Псевдомембранозный колит
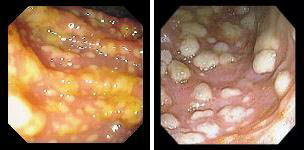
2. Сальмонелезный колит 3. Ишемический колит
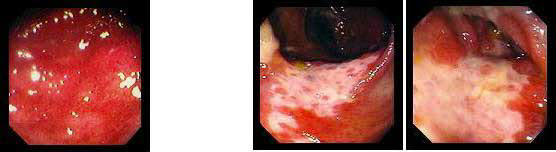
4. Солитарная язва прямой кишки
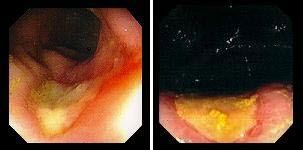
Наиболее сложен дифференциальный диагноз между язвенным колитом, болезнью Крона.
Болезнь Крона
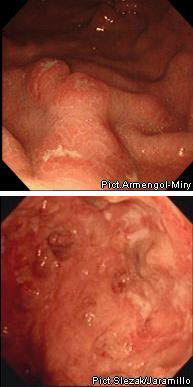
НЯК
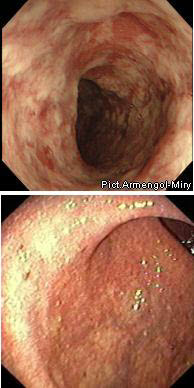

В 15-20% случаев не удается с уверенностью различить НЯК и болезнь Крона. В таких случаях применяется термин «неуточнённый колит».
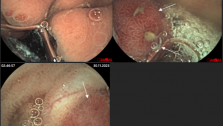
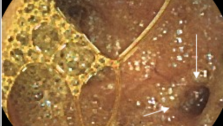
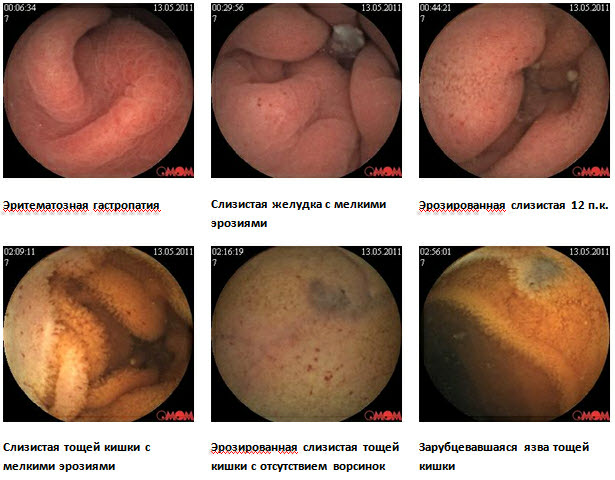
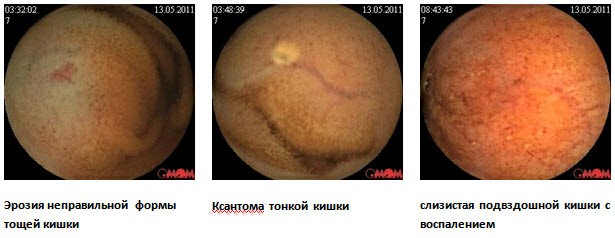
Клинический случай болезни Крона тонкой кишки с применением в обследовании методики капсульной эндоскопии
Больная Н., 61 год, находилась на обследовании в проктологическом отделении Киевской областной клинической больницы с диагнозом при направлении Неспецифический язвенный колит
Из анамнеза: болеет около 5 лет, когда начали беспокоить боли в животе, частый жидкий стул 2-
Для уточнения диагноза рекомендована капсульная эндоскопия. При обследовании: слизистая желудка диффузно гиперемирована, с мелкими эритемами. Слизистая тощей кишки с сегментарным поражением мелкими эрозиями, бархатистость местами снижена. В подвздошной кишке мелкие эрозии, язва округлой формы без признаков кровотечения, в терминальном отделе слизистая гиперемирована. Заключение: болезнь Кронатонкой кишки. С учетом клинических данных пациентке назначена диета, месалазин перорально и в микроклизмах, глюкокортикоиды, иммуносупрессоры, антибактериальная терапия.
Мониторинг клинической эффективности: незначительное улучшение уже через 5 дней, что выразилось в ликвидации болевого синдрома. Через 2 месяца больная прибавила в весе 5кг, стул нормализовался-1-2р/сут, оформленный, без патологических примесей, отмечает значительное улучшение качества жизни.
Смотреть также лечение неспецифического язвенного колита (НЯК).